Here we’ll outline an IT band syndrome treatment plan to help get you moving pain-free again.
IT band syndrome plagues the outside portion of the knee and is one of the most common forms of knee pain. The problem usually arises as an overuse injury, especially after ramping up the number of knee bends in a day. The obvious culprits are running and biking, but those aren’t the only activities that suddenly spike in volume. Jumping into a workout plan with more squats and lunges than you’ve done in a lifetime, or rolling out of bed and deciding it’s a good day for some serious hiking, are other examples of ways you might make your knee cranky.
The symptoms are usually subtle or non-existent to begin. Many runners say they’re able to start their runs pain-free, but shortly into it, a sharp pain develops to the side of their knee — the feeling of being stabbed by a knife.
Many assume it’s an issue coming from tightness, prompting stretching and foam rolling of the outer thigh. This idea was once strongly supported by articles and videos on “breaking up trigger points” or “releasing” the IT band from professionals on the internet. As of late, there has been an outcry against this form of treatment, since it doesn’t do much (although we’ll show you later that it still may be helpful.)
What the evidence has found is that the IT band is much too dense to make it softer or longer. Rubbing on your thigh isn’t harmful and probably feels good while you’re at it, but unfortunately, it’s not tackling any underlying issues and is, therefore, not much of a long-term fix.
In this article, we’ll take a good look at the science on IT Band Syndrome and hopefully give you some confidence to get around it.
ANATOMY & FUNCTION OF THE IT BAND
A general anatomy refresher on the knee will make this article a bit clearer. You can do that here in The Quick Guide to Understanding How Your Knee Works.
Taking it a step further, examine the IT band, or more precisely called the iliotibial band.
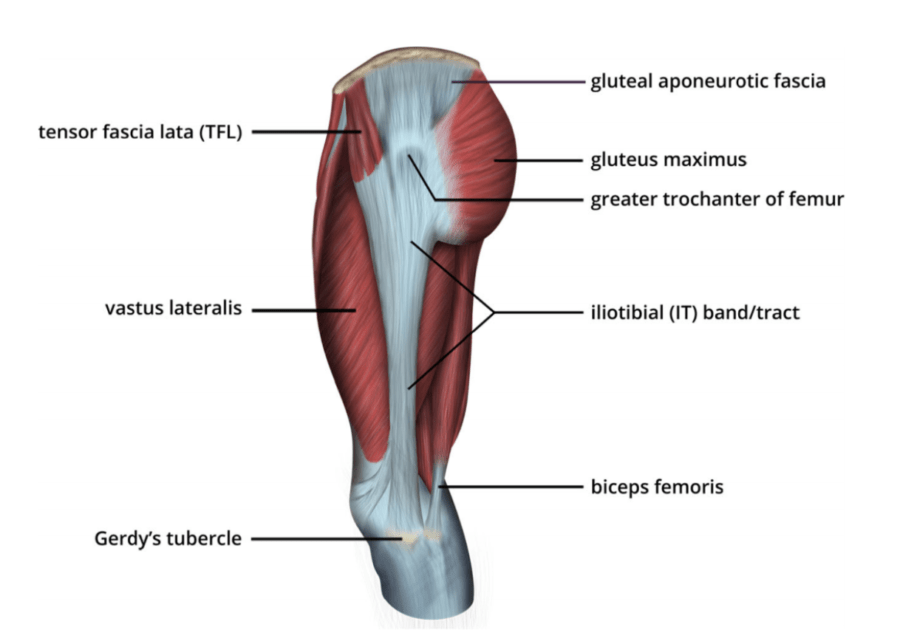
It’s a thick band of fascia, that intertwines with other fascia starting along the crest of the hip. It then runs along the outside of the leg where it finally attaches to the outer portion of the knee. Along the way, it’s a connecting place for the tensor fasciae latae, or TFL for short, on the front side, and the gluteus maximus muscle on the backside.
It covers a lot of distance, spanning both the hip and knee joint, leading many to assume any pain along the outside of the hip or thigh is some form of IT Band Syndrome. But those are different problems.
IT Band Syndrome a condition tied to a pinpoint spot outside the knee where the IT Band runs over a bony place called the lateral femoral condyle. The long-held belief is that irritation was coming from the IT band rubbing over this bony notch, but now we aren’t so certain (ref).
A 2006 study introduced evidence that the IT band is anchored down too well to roll around and get hung-up on things. Instead, they believed the irritation was more likely from a fat pad, a bursa, or other connective tissue getting compressed under the IT band (ref).
A later study partly refuted this. Saying the IT band does roll along the outside of the knee but didn’t conclude either way if it was an issue of friction or compression (ref). Surprisingly this is where we stand on the IT Band after more than a decade of research.
Regardless of the underlying problem, unless you’re looking to cut something out, you’ll approach it the same way.
DIAGNOSIS
Before we get too carried away, it’s a good idea to determine if IT Band Syndrome is what you’re dealing with.
It’s usually a straightforward diagnosis rarely requiring imaging or even special tests. Pain in the right spot, paired with a recent increase in activity, and no injuries to the knee, point to IT band syndrome. But there are other issues, like the strains to the LCL or a meniscus tear, that may present as an IT band issue. Our Red Flag Screen is a good evaluation of these other major issues. Reach out at support@crossoversymmetry.com and we’ll walk you through it.
Unfortunately, the treatment may be lengthy, but with active participation— things like activity modification, stretching, and strengthening— most are able to navigate the issue without any advanced treatment.
IT BAND SYNDROME TREATMENT
Here’s your game plan to help treat IT band Syndrome.
Rest
I’m sorry to say…this will require rest. It’s the four-letter word that every endurance or workout junkie hates to hear. They also happen to be the ones who will get IT band syndrome.
The unfortunate truth is that stopping provocative activities, like running and cycling, is the most important criterion to calm it down. An interesting side note related to rest and chronic use injuries like IT band syndrome is that many times surgical procedures work simply because it forces the issue of rest.
Start with a timeline of 2-weeks off from running, biking, or anything else that involves repeated flexion and extension of the knee. If you’re looking to get your cardio fix, give swimming a try. Or some runners find that they can bike without provoking symptoms.
After 2-weeks off evaluate the progress and your ability to move forward.
The downtime is relatively easy to navigate and fill with other activities. The real problem and where many hit setbacks is the return to activity.
The usual story is a dedicated runner starts struggling with knee pain. They take time off and do all the rehab stuff, then excitedly wake up one morning feeling better than ever. The happy ending is then ruined when they pick up right where they left off and piss off their knee again.
It’s important to return to activity through graded exposure. After 2-weeks off, take another 2-weeks as an on-ramp to getting back to where you once were. This helps reacclimate the tissues to stress and helps you gauge what you’re truly ready for. Just hit the eject button if you feel things get worse.
Pain Management
Most people with IT band syndrome have mild discomfort throughout the day. Simply backing off activity is probably the best way to deal with the pain issue.
Still, some might find it restricts them from activities and disrupts their rest. In this case, NSAIDs may be useful to fight off pain. But when returning to activity, logic would say it’s best to see how the body responds without any pain inhibitors.
Then for the last resort, corticosteroid injections may be considered, and that’s really only if visible swelling is present.
The Rehab Plan
Unfortunately, there is no definitive cure to IT band syndrome other than time to allow things to calm down. Still, additional work may help speed the process and keep pain from returning later on.
There are two main theories behind the treatment strategies. Tackle the IT band itself or the things that work closely with the IT band.
For the former, your IT band is not going to change by your own doing. The IT band is a thick fibrous strap of tissue, akin to a steel cable running down your thigh. Any effort to stretch, mash, or strengthen won’t change your IT band (ref).
What you can change are the muscles that tension the IT band and your biomechanics. The following are the common exercise recommendations to help fix your knee issue.
Runner’s Program for IT Band Syndrome
Our 30 Day Knee Fix helps guide this graded exposure with activity restrictions that progress over the one-month program. Here are our recommendations for runners dealing with knee issues:

Along with this, it’s advisable to avoid running hills, on grades that slope across your body (where one side is higher than the other, like as a shore of a beach,) and lots of tight turns.
Additionally, you don’t have to try hard to find recommendations for changing your footwear. This includes everything from getting fitted for the latest in shoe technology to going barefoot on your runs. There’s no real evidence to support this as a reliable cure, but don’t discredit that a worn-down cushion beneath your foot may be altering your gait and a reason why your knee is flaring up.
FOR PAIN RELIEF: MASSAGE, STRETCHING, AND TRIGGER POINTS
The first focus is on exercise tools that will get your pain to go away faster.
Lessening pain is largely about modifying the inputs being sent to the brain that are signaling there’s a problem. You’re already doing it by taking some time off from your provocative activities (running, ect.), but stretching and massage work can further your recovery.
Stretching
Going back to IT band anatomy, the tensor fascia lata (TFL) and glute max both pull on the IT band. Thus, helping these muscles to relax and lengthen, would reasonably help to unwind a taught IT band.
Here are two stretches to add to your routine, specifically working on the glutes and TFL:
Massage
I’m using the term massage to cover all forms of smashing to change your tissue. Again, the focus isn’t to fix your IT band but to change the environment around the IT band.
For basic deep tissue massage, there is a low level of evidence for the role of massage in dealing with pain. Not saying that it doesn’t work, it just lacks robust research to say that it’s a slam dunk (ref). Yet a massage is generally a relaxing experience, which is useful for managing pain (ref).
A more effective type of massage for loosening tight hip muscles combines pressure with joint movement (ref). It’s worth mentioning that you might feel loose and limber when you get off the table, but those benefits won’t likely extend throughout the day. So it can be a helpful tool but works best with other things to back it up. We’ll get into those in the strengthening section.
For a cheaper option, give your foam roller a try, even if it’s been blasted on the internet lately. Indeed, your tube of foam won’t soften or lengthen your IT band, but it may help to loosen up your tight hips (ref). If anything, it’s cheap, easy, and makes you feel good. As mentioned earlier, dealing with pain is about changing messages to the brain from bad to good ones, and a little roll-out can do that.
What about trigger points?
This is a loaded topic we won’t dive into, but we’ll skim the surface because it’s bound to come up if you talk to anyone about your knee pain.
Not too long ago, the term trigger point went mainstream to explain how little tender spots in the body were knotted pieces of muscle and fascia. Even more, those little buggers might be making things hurt elsewhere. For example, trigger points in your hips may be passing notes to your brain saying there is a problem down at your knee.
Although, the myofascial release train went faster than the evidence to support it. Where we currently stand is we know about as much on trigger points as we do IT band syndrome. It seems to be something real, with many theories to explain it, but no silver bullet.
I don’t want to discourage things that fall under the header of “breaking things up.” Just be wary of anything promising instant cures in exchange for all your money.
THE NEED FOR STRENGTHENING
The cornerstone of just about any IT band rehab plan is strengthening the hips. Although, a 2015 review on the many studies attempting to link strength and mechanical issues to lateral knee pain shows nothing exciting (ref).
This questions if exercises will actually fix anything. The best answer is no one truly knows, but it’ s probably still worth the effort.
First of all, even the strongest athletes with perfect mechanics get injured if workloads progress quicker than they’re ready. A study of over 1000 soldiers who undertook a preventative exercise program designed to reduce knee and shin injuries showed no significant reduction in IT band Syndrome (ref). You’ll find similar results in a recent study of runners who completed a strengthening program alongside training for the New York City Marathon (ref).
Despite preventative measures, it seems that a 10% injury rate is inevitable for endurance activities due to errors in progression. And in every random sample of activity participants, a few take steps too big as they go through their program.
In regards to biomechanics, movement at the hip and ankle is tied to the size and direction of forces at the knee. At this point, we don’t know if it’s the IT band getting irritated, or if it’s tissues getting impinged underneath. Regardless, lessening the strain on the IT band is a logical target for addressing the issue either way.
The IT band creates lateral stability at the knee to keep it from caving or rotating inwards. You can better support the IT band by developing strong hip muscles to keep the leg centered under the body (which also helps with other running issues.) We talk about this extensively here: The Big Risk Factor for Running Injuries.
The lack of evidence may also be an issue of strengthening protocol. It’s one thing to isolate little muscles, it’s another to challenge strength and stability for the long haul. For an athlete, this requires more than just a little booty burn. It should be a challenging stimulus that requires the body to maintain stability as you fatigue.
The worst-case scenario is that it doesn’t do much for your knee pain, but you’ve got stronger and better-defined legs as part of your rehab.
Lastly, a strengthening plan fits alongside graded exposure, which as you remember, is your gradual return to activity. Exercises that keep the hips and core muscles firing, without provoking your knee pain can help you progress back to running again.
With time and a little bit of patience, you will most likely fix this issue without needing any further help. If you have any questions, please reach out to me at matt@crossoversymmetry.com.
SUMMARY: IT BAND SYNDROME TREATMENT PLAN
- Relative Rest for at least 2-weeks. Then gradually reintroduce activity, but back it off if you have pain.
- Foam roll ITB and vastus lateralis
- Stretch Glutes, TFL, hip flexors, calves
- Work on strengthening the hip abductors and external rotators (particularly gluteus medius)
If you need help with this, our Hip & Core System can help guide your rehab. It includes both our Hip & Core Band and a 30 Day Knee Fix will help to lay out a plan. Click here for more info…


